A midwife providing care to a pregnant woman in Nigeria. Image Credit| World Health Organization African Region
Introduction
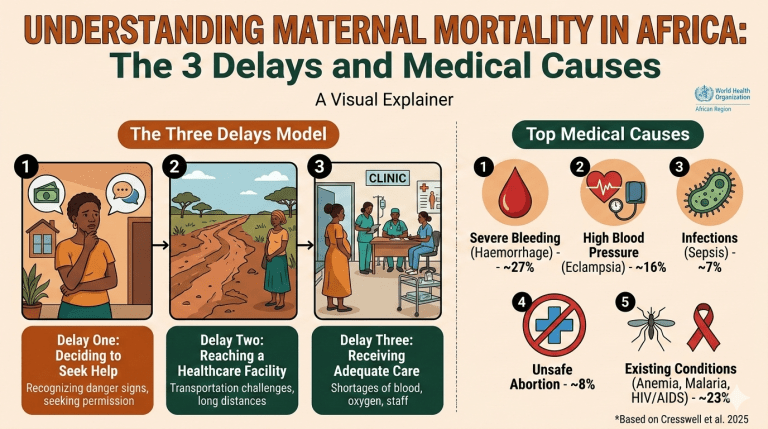
Maternal mortality from pregnancy emergencies in many parts of Africa follows a typical, dangerous pattern. Imagine a woman who starts labour at 4 AM. By the time she gets permission from her family to seek help, several hours have passed. Because she lives 20 kilometers from a clinic and cannot afford a taxi, she waits even longer for transport. By the time she reaches a hospital, often hours later, the facility may lack the equipment, nurses and doctors needed to attend to her. This sequence of events is so common that researchers have a name for it: The Three Delays of Maternal Mortality.
These delays, in addition to several medical conditions, healthcare system gaps, and and social and economic barriers, are the causes of high maternal mortality in Africa.
What Is Maternal Mortality?
Maternal mortality is the death of women resulting from complications during pregnancy, childbirth, or non-accidental events 42 days after delivery (1). A maternal death is called ‘late’ when the death occurs following 42 days of delivery but within one year after the pregnancy ended, and this death must be related directly or indirectly to the pregnancy or childbirth process.
A direct maternal death is a death caused by situations arising from the pregnancy, labour, or caesarean section. For instance, severe bleeding and infection. Indirect maternal death, on the other hand, means death from an already existing health condition worsened by pregnancy or labour, like heart or kidney disease (1).
Recent Data on Maternal Mortality in Africa
In 2023, about 260,000 women died during pregnancy or childbirth worldwide (2). Of these deaths, 182,000 happened in sub-Saharan Africa (2). This means Africa had 70% of all maternal deaths in the world in 2023 (2).
According to the numbers released by the United Nations Children’s Fund (UNICEF), a woman living in Western Europe has a 1 in 14,000 chance of dying from pregnancy (3), but in sub-Saharan Africa, the chance is 1 in 55 (3). This means that African women are 250 times more likely to die from pregnancy than European women.
Every single day, an estimated 487 African mothers die from preventable causes (4). That is 487 families losing a mother, wife, sister, or daughter, and 487 children who will grow up without their mother.
In 2023, Africa’s maternal mortality ratio (MMR) was 442 deaths out of 100,000 live births as opposed to 727 deaths in the year 2000 (4). This 40% decline over 23 years is a good improvement; however, it’s still lagging behind.
Based on the target set by the United Nations, maternal mortality should be below 70 deaths out of 100,000 births everywhere in the world by 2030 (2). But at the current rate of improvement, Africa will only achieve 350 deaths per 100,000 births by 2030 (4). This is five times higher than the set target.
A 2023 study released by the World Bank revealed that 692 mothers died for every 100,000 babies born in South Sudan, 784 died in Chad, and 993 died in Nigeria (5). These are very high numbers compared to European countries, where only 10 mothers die out of 100,000 live births (2).

Causes of Maternal Mortality in Africa
Maternal deaths in Africa rarely happen because of one problem, but mostly when a medical emergency meets systemic barriers.
Serious medical conditions like heavy bleeding, high blood pressure, infections, unsafe abortions, and illnesses such as malaria or anaemia can quickly become life-threatening. But they often become more deadly when they meet what experts call the Three Delays of Maternal Mortality.
Understanding this dangerous combination helps explain why the crises continue and how to effectively manage them.
Click here to read the full article on the Causes of Maternal Death in Africa.
Why Maternal Mortality Remains High in Africa
Several factors contribute to the high number of maternal deaths in Africa. These factors include the following:
I. Healthcare System Failure
Most maternal deaths in Africa are preventable. A woman should not die from bleeding if the hospital has blood; neither should a woman die from high blood pressure if the hospital has the right drugs or enough trained staff.
The following elements make up the healthcare system failure that leads to maternal death in Africa:
- Insufficient Healthcare Workers
In high-income countries, skilled health workers attend 99% of births (2); however, in low-income countries, only 73% of births have skilled attendance (2).
In some rural areas of Africa, the number of patients outnumbers the available trained nurses and doctors. This leads to people not receiving the care they need, and when they do receive the care, it is not enough.
- Poor Infrastructure
Delivering optimal healthcare to pregnant women and women in labour requires both manpower (nurses, doctors, etc.) and materials.
However, many African health facilities lack the basic resources essential to caregiving and treatment.
- Weak Referral Systems
When a small health centre cannot handle an emergency, it should send the patient to a bigger hospital. This is called referral. However, most African countries experience broken referral systems because of the absence of ambulances to transport patients, poor communication between hospitals, and no standardised procedures for emergency referral.
Hence, women die during transfer or while waiting for the transfer to happen.
II. Insufficient Funding
In many African countries, the health sector gets very little financial allocation from its government.
Due to this insufficient allocation of funds, a lot of African countries depend on external donors for a significant proportion of their health funding. So, when the United States and the United Kingdom cut their health aid to Africa in 2025, many maternal health programmes collapsed.
This collapse in maternal health programmes meant less treatment options, significantly increasing maternal mortality in Africa.
III. Geographic Inequality
Women in urban areas have much better access to healthcare than women in rural areas.
A woman in Nairobi (the capital of Kenya) can reach a well-equipped hospital in 30 minutes, while a woman in rural northern Kenya might take 2 hours to get to a health facility. The higher the distance, the higher the chance of not accessing good care, hence increasing the risk of maternal death.
More than 60% of African countries now report that over 80% of births have skilled attendance (4). But this hides a problem: the remaining 20%, who are mostly rural and poor, are facing the risk of not accessing care when they need it.
IV. Poverty, Teenage Pregnancy, and Child Marriage
Poverty is a socioeconomic condition that increases the risk of maternal death in Africa (6).
This is because poverty creates a perfect combination of unfavourable conditions that limit access to care, interfere with health-seeking behaviour, and predispose women to poor health conditions like anaemia and malaria.

Teenage pregnancy and child marriage further expose young girls to maternal death. In many parts of sub-Saharan Africa, more than 50% of girls start having children before age 19 (6).
These teenage mothers face much higher risks of death than adult women because of the following:
- An undeveloped pelvis (hip bones), which might be too small for childbirth
- Higher risk of complications
- Less access to care during pregnancy
- Violence from partners or family members who are angry about the pregnancy
- No decision-making power regarding when and how to seek care
Related: Why Neglected Tropical Diseases in Africa Remain Underfunded
African Countries That Made Progress in Reducing Maternal Mortality
Irrespective of the high number of women who die from pregnancy and childbirth in Africa, some African countries have made remarkable progress in saving mothers’ lives.
According to the data collected by WHO Africa from 2017 to 2020, six African countries achieved high reductions in maternal mortality (7). First is Sierra Leone, which led with nearly a 60% reduction, dropping from 1,120 deaths per 100,000 live births in 2017 to 443 in 2020. Tanzania followed with a 55% reduction, Eswatini achieved a 45% reduction, and Mauritania reduced maternal deaths by 39%, while Ethiopia and Eritrea each achieved a 33% reduction (7).
Tanzania’s success came from expanding emergency obstetric and newborn care centres, implementing a national maternal and perinatal death review system, and providing an emergency transport referral system where taxi drivers act as ambulances in rural areas. Ethiopia deployed health extension workers to remote areas and built maternity waiting homes where pregnant women from distant villages could stay near hospitals before delivery.
These countries prove that maternal deaths can be prevented when governments make it a priority.
How To Further Reduce Maternal Mortality In Africa
To save African mothers from dying from pregnancy and childbirth, here are five things that can make a difference:
1. Increase Skilled Birth Attendance
Every birth should have a trained midwife, nurse, or doctor present.
African countries need to:
- Train more midwives and send them to rural areas
- Pay healthcare workers properly so they do not leave for other jobs
- Build maternity facilities in every district
2. Strengthen Emergency Obstetric Care
District hospitals in Africa should be able to:
- Perform emergency surgeries
- Give blood transfusions
- Treat severe bleeding
- Treat pre-eclampsia and eclampsia
- Treat infections
This requires equipment, medications, trained staff, reliable electricity and water.
3. Improve Transportation and Referral Systems
African governments and health policymakers need to:
- Provide ambulances in every district hospital
- Build and maintain roads to rural areas to ease access and referral
- Create communication systems between health facilities
- Establish clear referral protocols
4. Address Social and Cultural Barriers
African communities need:
- Education about pregnancy danger signs
- Campaigns to combat stigma and traditional beliefs that prevent women from seeking care
- Programs to empower women to make their own healthcare decisions
- Efforts to end child marriage
- Support for girls to stay in school
5. Increase and Sustain Funding
African governments need to:
- Allocate more budget to maternal healthcare
- Provide free or subsidized maternal healthcare
- Invest in health infrastructure (hospitals, equipment, ambulances)
The Cost of Maternal Mortality in Africa
The death of a mother in Africa creates a long-term gap in families, communities, and in the country as a whole. These gaps have developmental, social, and economic impacts.
Children who lose their mothers are less likely to go to school and more likely to suffer malnutrition, live in poverty, face abuse or die before age 5.
Communities that lose their women and mothers to death have lost primary carers who contribute to communal productivity, economic growth and social stability.
Conclusion
A good number of women who die from pregnancy and childbirth would have lived if their communities were empowered to prioritize their health. If mothers had the power to make their own decisions, they would not wait hours for permission to seek help. If roads were better and hospitals were equipped with trained staff and resources, these lives could be saved.
Every single systemic failure that kills mothers in Africa is preventable. We already know the social and economic solutions that work. What we lack is the political will to invest in them.
Until African governments prioritize maternal healthcare by investing in hospitals, improving roads, and empowering women, mothers will continue to die from causes we know how to stop.
References
1. World Health Organization. Maternal deaths [Internet]. Geneva: World Health Organization; 2026 [cited 2026 Feb 24]. Available from: https://www.who.int/data/gho/indicator-metadata-registry/imr-details/4622
2. World Health Organization. Maternal mortality [Internet]. Geneva: World Health Organization; 2025 Apr 7 [cited 2026 Feb 24]. Available from: https://www.who.int/news-room/fact-sheets/detail/maternal-mortality
3. UNICEF. Maternal mortality rates and statistics [Internet]. New York: UNICEF; 2025 Apr 9 [cited 2026 Feb 24]. Available from: https://data.unicef.org/topic/maternal-health/maternal-mortality/
4. World Health Organization. Regional Office for Africa. African region’s maternal and newborn mortality declining, but progress still slow [Internet]. Brazzaville: World Health Organization; 2025 Apr 7 [cited 2026 Feb 24]. Available from: https://www.afro.who.int/news/african-regions-maternal-and-newborn-mortality-declining-progress-still-slow
5. World Bank. Maternal mortality ratio (modeled estimate, per 100,000 live births) [Internet]. Washington (DC): World Bank Gender Data Portal; 2026 [updated 2026 Feb 5; cited 2026 Feb 24]. Available from: https://genderdata.worldbank.org/en/indicator/sh-sta-mmrt
6. Rodriguez L. Why maternal mortality is so high in sub-Saharan Africa [Internet]. New York (NY): Global Citizen; 2021 Aug 6 [cited 2026 Feb 25]. Available from: https://www.globalcitizen.org/en/content/maternal-mortality-sub-saharan-africa-causes/
7. WHO Africa. Maternal mortality regional fact sheet [Internet]. Brazzaville: WHO Regional Office for Africa; 2020 [cited 2026 Feb 2]. Available from: https://files.aho.afro.who.int/afahobckpcontainer/production/files/iAHO_Maternal_Mortality_Regional_Factsheet.pdf